Thyroid Cancer :
About Thyroid Gland
Thyroid is gland having shape like a small butterfly with right and left Lobe connected by a narrow piece of gland known as Isthmus. Thyroid gland is located in the front part of the neck and plays a major role in controlling body’s metabolism. It also liberates the hormones that controls many functions in the body like using the energy, producing body heat, and consumption of oxygen. Thyroid gland also regulate a person’s metabolism, blood pressure, heart rate and body temperature.
Thyroid Cancer
Thyroid cancer occurs when the cells mutate or alter. The abnormal cells starts to multiply in your thyroid and when they grow beyond control, they form a tumour. Thyroid cancer is one of the treatable cancers, If it’s detected in the early stage.
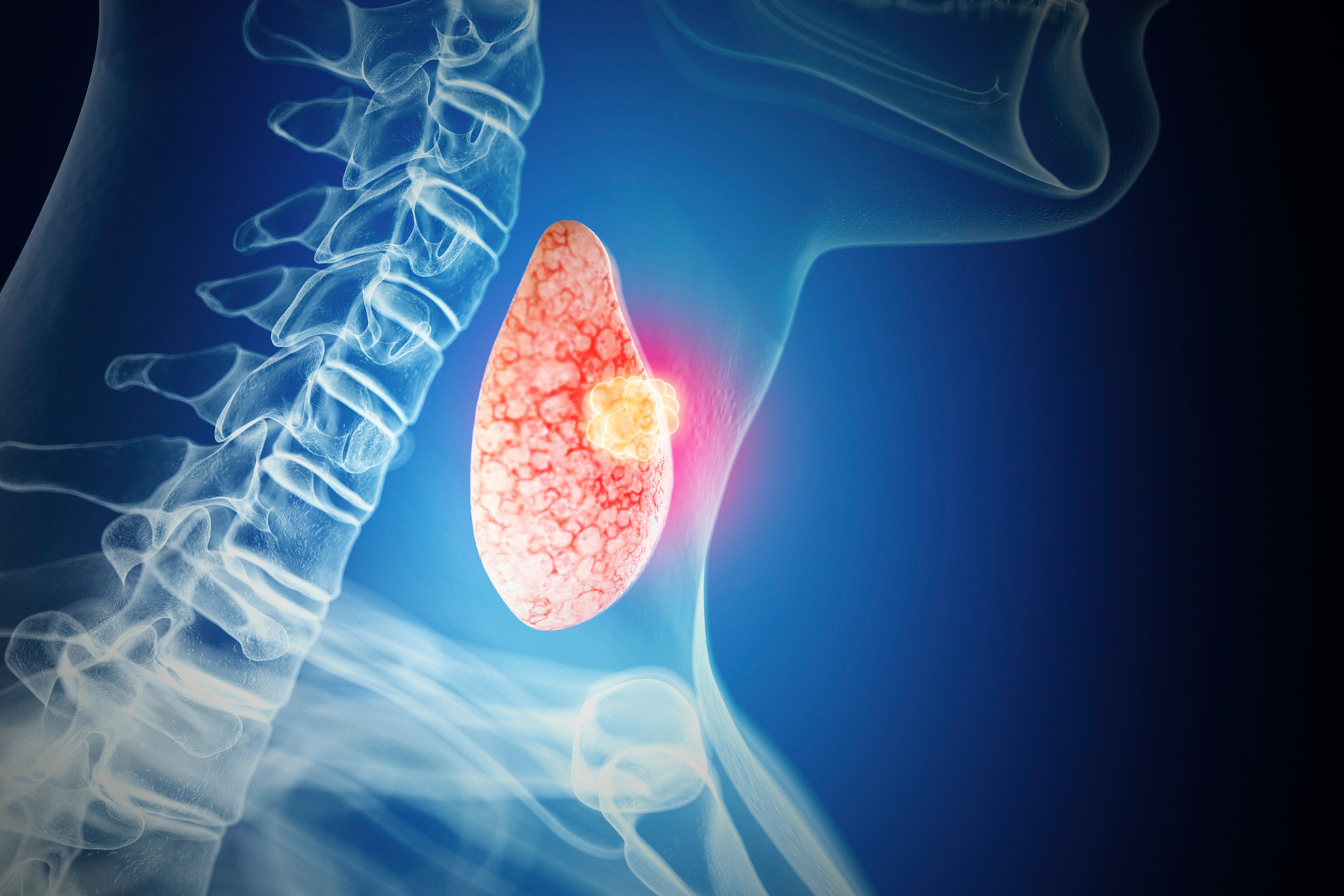
Types of Thyroid Cancer :
Papillary thyroid cancer :
Papillary Thyroid Cancer are also known as Papillary Carcinomas or papillary adenocarcinomas. About 80% of thyroid cancers are papillary cancers. The growth of Papillary Thyroid Cancer is very slow and normally occur only in one lobe of the thyroid gland. Though the growth of these cancer is slow, the papillary cancers broaden up to the lymph nodes in the neck. Papillary Thyroid Cancers are not that fatal though they have spread to the lymph nodes and also can be treated successfully.
Follicular Thyroid Cancer :
Follicular Thyroid cancer is one of the most common type of cancer which can occur in 1 out of 10 thyroid cancers. This cancer if found commonly in those countries where people lack iodine in their diet. Follicular Thyroid cancer rarely spread to lymph nodes, but can widely spread to other parts of the body, like the lungs or bones and also tend to spread into the blood vessels. The prognosis for follicular Thyroid cancer is not much satisfactory as compared to Papillary cancer.
Medullary Thyroid Cancer/Medullary thyroid carcinoma :
Medullary Thyroid Cancer (MTC) is found in 4% of thyroid cancer cases. Medullary thyroid cancer grows from the Cancer cells of the thyroid gland, which produce a hormone called Calcitonin. This hormone helps to balance the amount of calcium in blood. Sometimes Medullary Thyroid Cancer may extend to the lymph nodes, the lungs, or liver even before a thyroid nodule is discovered. This class of thyroid cancer is much very to find and treat.
There are two types of Medullary Thyroid Cancer:
Anaplastic thyroid cancer :
Anaplastic carcinoma is an uncommon type of Thyroid cancer which sometimes grows from an existing papillary or follicular cancer. Anaplastic carcinoma is also called as Undifferentiated Carcinoma as the cancer cells do not appear like normal thyroid cells. This cancer time and again spreads fast into the neck and to other parts of the body, and is very hard to treat.
Parathyroid cancer :
Four tiny glands called as Parathyroids are attached behind but to the thyroid gland. The parathyroid glands help to balance the body’s calcium levels.
Parathyroid cancers makes a person very weak, tired, and drowsy. It can also lead to high urination which can cause dehydration. This can worsen the weakness and drowsiness of the patient. Other symptoms include pain from kidney stones, bone pain and fractures, constipation, and depression.
Larger parathyroid cancers may also be detected in the form of a lump near the thyroid. If the lump is too large, then it can be removed only through Surgery. Parathyroid cancer is quiet difficult to cure as compared to Thyroid cancer. Parathyroid cancers are very uncommon.
TNM system for thyroid cancer :
Cancer staging describes how large a cancer is, and the degree to which the disease has spread. The staging guidelines developed by the American Joint Committee on Cancer (AJCC) are often used to stage thyroid cancers.
Cancer staging illustrate the size of the Cancer, and the extent of the spread of the disease. The staging guidelines developed by the American Joint Committee on Cancer (AJCC) are often used to stage thyroid cancers.
TNM system for thyroid cancer.
The stages are based on three categories:
Tumour (T) :
In the TNM system, the letter “T” along with a letter or number (0 to 4) explains the size and location of the tumour. Tumour size is measured in centimetres (cm). A centimetre is counted equal to the width of a standard pen or pencil.
In the Cancer staging, “T” in thyroid cancer, doctors may subdivide the general categories by adding the letter “s” to indicate a solitary (single) tumour or “m” to indicate multifocal (more than 1) tumours.
Node (N) :
The “N” in the TNM staging system stands for lymph nodes. Careful evaluation of lymph nodes is an important part of staging thyroid cancer. There are many regional lymph nodes located in the head and neck area. Lymph nodes in other parts of the body are called distant lymph nodes.
Metastasis (M) :
The “M” in the TNM system describes whether cancer has spread to other parts of the body, called distant metastasis.
Stages of Thyroid Cancer :
The thyroid cancer staging classification system is very similar for older patients with differentiated tumours and for those with medullary thyroid cancer. Age is not a consideration when classifying medullary cancers.
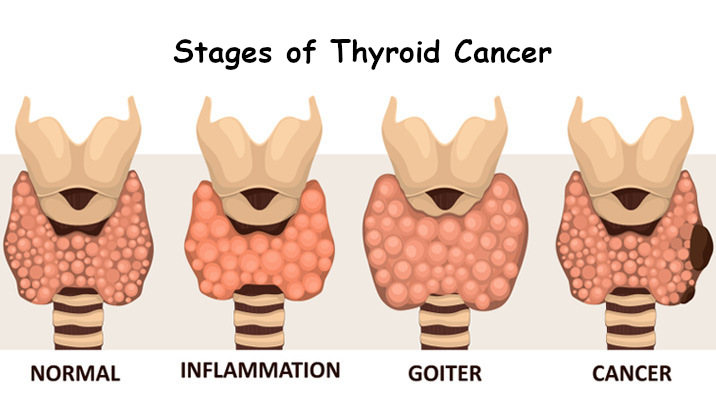
STAGE I (stage 1 thyroid cancer):
STAGE II (stage 2 thyroid cancer):
The cancer meets one of the following criteria:
STAGE III (stage 3 thyroid cancer):
The cancer meets one of the following criteria:
STAGE IV (stage 4 thyroid cancer) :
This is the most advanced stage of thyroid cancer, is further subdivided depending on where the cancer has spread:
Stage IV anaplastic thyroid cancer (stage 4 anaplastic thyroid cancer) :
Anaplastic/undifferentiated thyroid cancers are much more aggressive than the other subtypes and are all considered stage IV:
Recurrent Thyroid Cancer :
Post the treatment for thyroid cancer, there are chances of redeveloping primary cancer which is called as recurrent disease. Recurrent thyroid cancer may occur years after the initial treatment for the disease is completed.
Recurrent thyroid cancer normally occurs in the neck region like the lymph nodes. This is called a regional recurrence. Some patients experience distant metastases, or cancer that has spread to other areas of the body. Distant thyroid cancer recurrence typically develops in the bones and lungs.
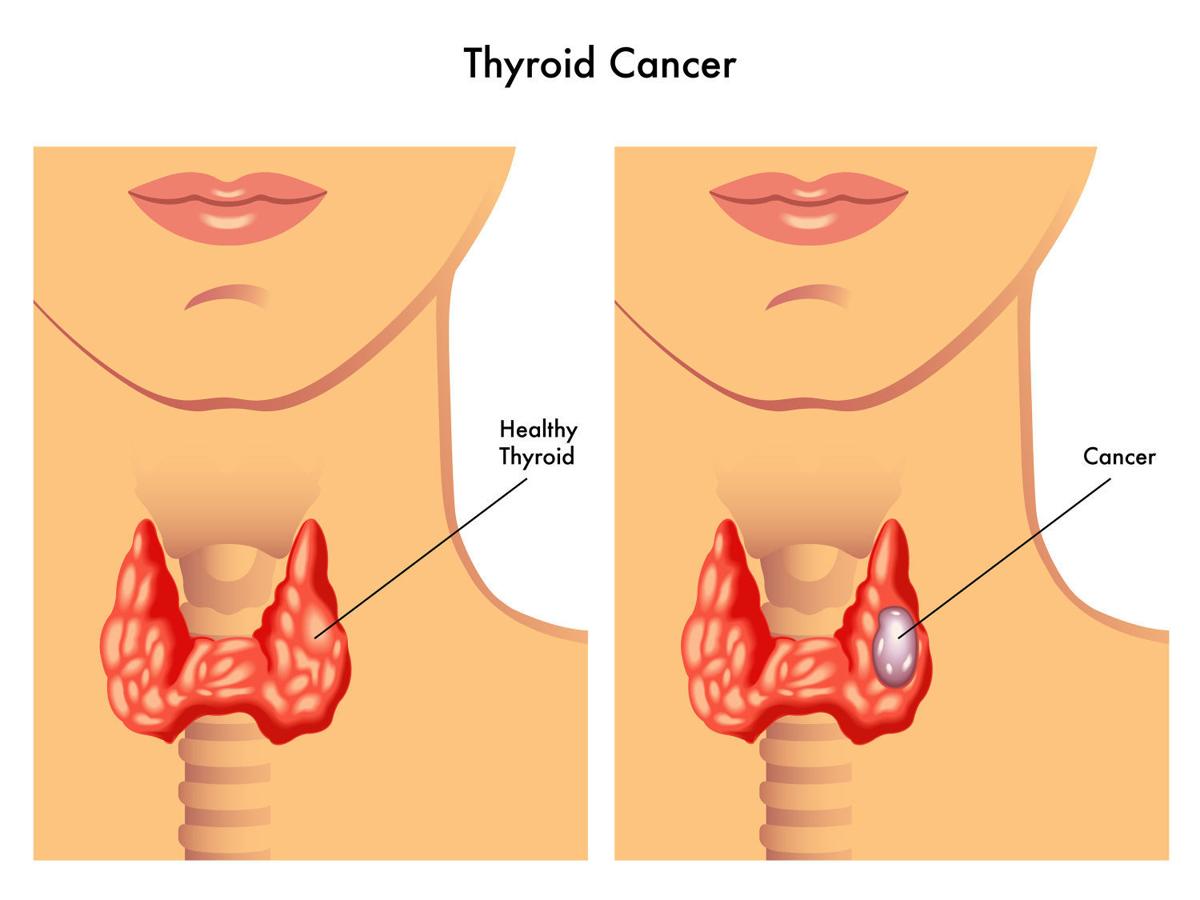
Symptoms of Thyroid Cancer :
Thyroid cancers are often diagnosed by routine examination of the neck during a general physical exam. They are also unintentionally found by x-rays or other imaging scans that were performed for other reasons.
At the time of general physical exam, Thyroid cancers are often detected by routine examination of the neck. While the performing of X-rays or other imaging scans for other causes, Thyroid Cancer are also accidently found during this process.
People with thyroid cancer may experience the following symptoms or signs. Sometimes, people with thyroid cancer do not have any of these changes.
The cause of a symptom may be a different medical condition that is not cancer.
These symptoms may be caused by thyroid cancer; other thyroid problems, such as a goitre; or a condition not related to the thyroid, such as an infection.
Other possible symptoms of thyroid cancer include:
Once the cancer is diagnosed, Palliative care or Supportive care plays an important role of cancer care and treatment. This care process starts immediately after diagnosis and is continued throughout treatment. During the Palliative care, if the patient experience any new symptoms or a change in symptoms, then they must inform the health care team about the same immediately.
Treatments for Thyroid Cancer :
Thyroid cancer is normally treated by 1 or a combination of treatments. Types of treatments used for thyroid cancer are based on the stage of disease.
Treatment options and recommendations depend on several factors, including:
Cancer treatment is generally given as per the guidelines prescribed by the panels of expert physicians. Although most thyroid cancer is curable, the doctors have different opinions in regarding the treatment of thyroid cancer, specifically pertaining to the combination of treatments to use and the timing of when treatments are done. Also, the treatment program depends on other factors like the stage, type, and progression of the cancer.
Common options for treating thyroid cancer include:
A) Chemotherapy:
Chemotherapy is sometimes used to sensitize anaplastic thyroid cancers to external beam radiation therapy (EBRT).
In chemotherapy, the possible side effects may include vomiting, nausea, mouth sores and even hair loss. Doctors care team may opt for multiple procedures which will help to reduce or moderate chemotherapy-related symptoms. Patients may receive pre-medications to make the pain more tolerable before giving the chemotherapy for thyroid cancer.
B) Hormone therapy:
In order to maintain bodies normal metabolism, daily hormone supplements is utmost necessary / mandatory for those Patients suffering from Thyroid cancer as almost all the thyroid glands are removed through the surgery.
Normal or above-normal levels of thyroid hormone in the blood have to be maintained which can help in reducing the percentage of thyroid stimulating hormone (TSH) made by pituitary gland.
TSH is a monitoring hormone that revitalize the development of the thyroid gland, and may also stimulate thyroid cancer cells. Generally, the pituitary gland produces more thyroid stimulating hormone TSH when levels of thyroid hormone are low, so increasing these levels can send a signal to reduce production of thyroid stimulating hormone, and potentially help to keep some thyroid cancers from recurring.
C) Radiation therapy:
Radiation therapy is an alternative for cancer treatment in which doses of radiation are used to destroy the cancerous cells and decrease tumours.
Radiation treatment options for thyroid cancer include:
External Beam Radiation Therapy (EBRT): This therapy throws a beam of radiation from outside the body at cancerous tissues residing inside the body.
Examples of EBRT include: - Stereotactic radiosurgery, 3D conformal radiation therapy, TomoTherapy® IMRT, and IGRT.
Specific advantages of EBRT for thyroid cancer may include:
D) Intensity modulated radiation therapy (IMRT):
Intensity Modulated Radiation Therapy (IMRT) uses advanced software to schedule a specific dose of radiation, as per the size of the tumour, shape, and location. Linear Accelerator, a computer-guided device supply radiation in marked doses that match the 3D geometrical shape of the tumour, which also includes the concave and complex shapes. IMRT may be an alternative for the patient who previously have taken radiation therapy for thyroid cancer and still are experiencing recurrent tumours in the treated area.
Intensity Modulated Radiation Therapy (IMRT) permits the radiation oncologists to use higher radiation doses than traditional therapies as compared to Standard Radiotherapy. Simultaneously, IMRT helps to save the surrounding healthy tissue from being affected by the harmful doses of radiation.
E) Radioactive iodine therapy:
Radioactive iodine therapy for thyroid cancer may be singly used or in combination with surgery. Usually, the whole of Iodine in the bloodstream is absorbed by the Thyroid Gland. Treatment with Radioactive iodine is used often for thyroid cancers that have spread to the lymph nodes and other parts of the body. In this procedure, the Radioactive iodine is discharged into the body through Liquid or by Capsule. The potential benefit of Radioactive iodine therapy is not clear though the patients with small tumours have undergone surgery for removal of the tumours.
Radioactive iodine therapy is prescribed only for differentiated cancers like papillary or follicular thyroid cancers. This treatment is not used for medullary or anaplastic thyroid cancers as these types of cancer cells do not consume iodine.
F) TomoTherapy®:
TomoTherapy® is combined form of intensity modulated radiation therapy (IMRT), with the accuracy of computed tomography (CT) scanning technology, in single machine. With the help of TomoTherapy® sensitive structures are avoided, delivering high precise radiation to match complex tumour shapes. TomoTherapy may reduce radiation exposure to healthy tissues and organs Using built-in CT scanning to confirm the shape and position of the tumour before each treatment,
TomoTherapy may offer the following potential advantage for thyroid cancer patients:
Surgery :
Surgery is the removal of the tumour and some surrounding healthy tissue during an operation, called a margin. Surgery may also be called a resection and is the important treatment for people having thyroid cancer.
Depending on the size of the thyroid nodule, common surgical options include:
Thyroid Hormone treatment:
Patients who have undergone thyroid Cancer surgery, normally are also given thyroid hormone therapy. As additional treatment to replacing the hormone that is needed by the body. The thyroid hormone medication may reduce the growth of any remaining differentiated cancer cells.
An Endocrinologist normally gives the Thyroid hormone replacement treatment to the Patient suffering from Thyroid Cancer. An Endocrinologist is the doctor who is specialized in treating problems related to the hormones, glands, and the endocrine system.


